When I stepped into the role of overseeing clinical operations for a teletherapy platform, I carried with me years of experience from college counseling center work. I lived with the same pressures counseling directors face every day: rising demand, increasing acuity, limited staff capacity, and the responsibility to deliver ethical, thoughtful care within institutional constraints.
At the same time, I spent enough time working alongside Student Affairs leaders to understand their reality as well. They are asked to make decisions about access, equity, resources, and outcomes — often without clear, comparable data across systems of care.
As online therapy expanded, it became clear that access alone was not the hardest part to solve. The harder question was how to extend care without losing the standards, language, and accountability that counseling centers have spent decades building.
For me, the question had never been whether teletherapy belongs within the ecosystem of offerings for college mental health. It was whether teletherapy could be delivered in a way that counseling directors would recognize as clinically sound — and that Student Affairs leaders could trust as institutionally responsive.
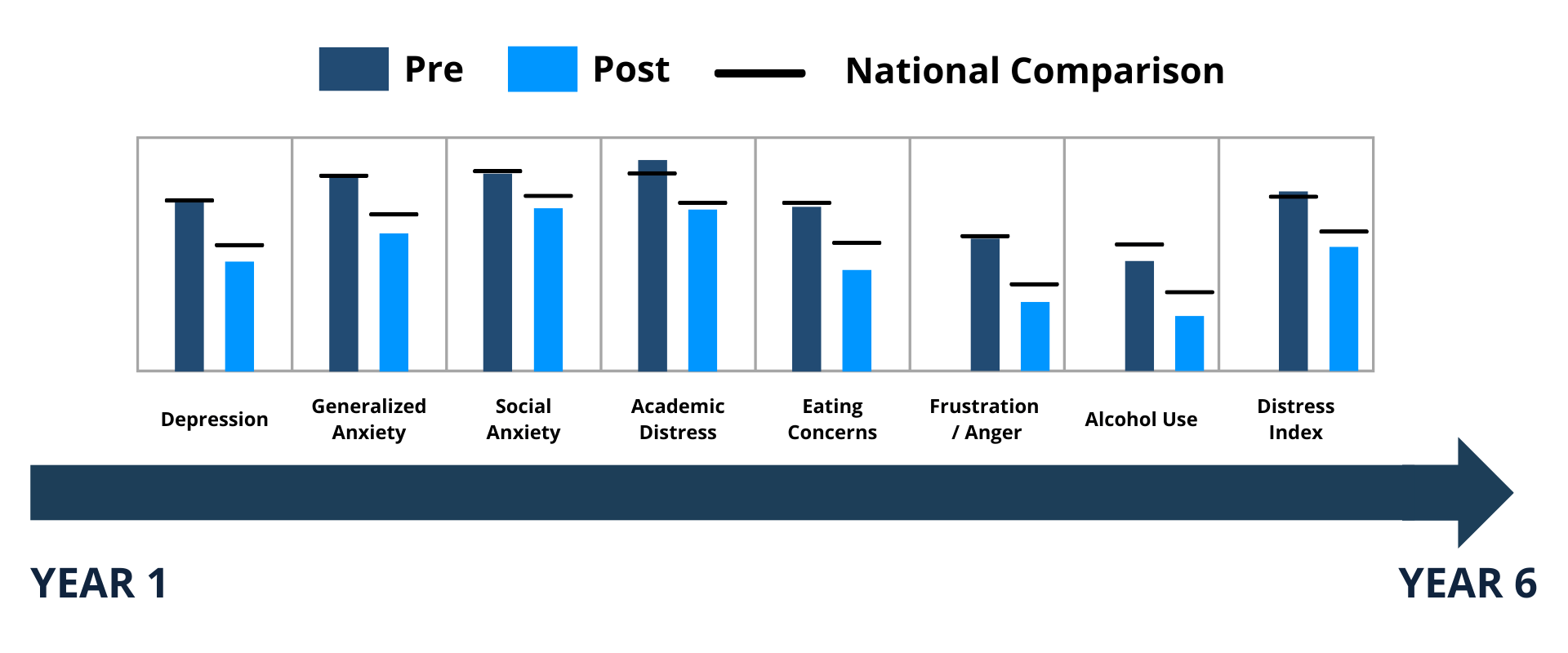
As a clinical leader who has worked inside counseling centers, as well as in clinics and private practice, I’ve seen how – when done well – assessment functions as more than a tool. It informs how clinicians understand complexity, how supervisors provide clinical support, and how institutions make resource decisions and maintain accountability to students and other stakeholders.
With the adoption of teletherapy use by institutions, the question hasn’t been whether access would expand — it has been whether standards could be preserved while doing so. Embedding CCAPS-34 into our assessment framework was a deliberate decision to ensure that online care spoke the same clinical language as campus care, rather than creating a parallel system.

![[Ongoing] Headshots](https://www.bettermynd.com/wp-content/uploads/2026/02/Ongoing-Headshots-scaled.png)